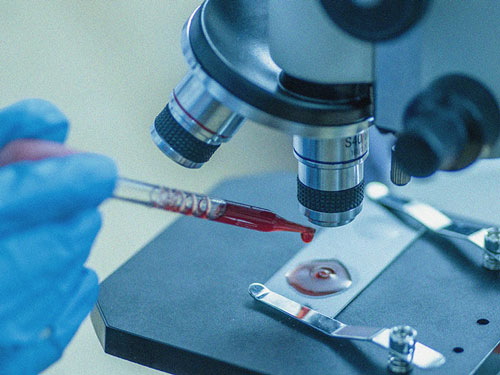
EXCESSIVE blood clotting is a recognized feature of severe Covid-19. But a new study suggests that some hospitalized patients may also be vulnerable to bleeding, which is associated with an increased risk of death.
After an injury, clotting prevents dangerous loss of blood. Blood clots, or “thrombi,” can also block blood vessels, however, with potentially fatal consequences.
Normally, our blood maintains a delicate balance between its tendency to form clots and its tendency to break them down.
In particular, the body does this by continually adjusting the activity of a protein in the blood called plasminogen, which promotes the breakup of blood clots, or “thrombolysis.”
Stay informed with live updates on the current Covid-19 outbreak and visit our coronavirus hub for more advice on prevention and treatment. The body performs this balancing act by changing the levels of two other proteins circulating in the bloodstream, known as tissue plasminogen activator (TPA) and plasminogen activator inhibitor-1.
As their names suggest, the former activates plasminogen and therefore promotes thrombolysis, while the latter has the opposite effect.
Early in the pandemic, research began to show that the blood of critically ill patients with Covid-19 is unusually “sticky” or prone to clotting, with potentially fatal consequences including deep vein thrombosis, stroke, and heart attack.
These findings led to the practice of giving high doses of anticoagulant drugs — which work in various ways to prevent the development of blood clots — to patients hospitalized with Covid-19 throughout their treatment.
However, a new study by researchers at Michigan Medicine and the University of Michigan in Ann Arbor suggests this may not be the best approach for all patients.
They measured levels of TPA and plasminogen activator inhibitor-1 in the blood of 118 patients hospitalized with Covid-19 as well as 30 healthy controls. They found very high levels of both proteins in the blood of these patients. These proteins were associated with respiratory difficulties, but high levels of TPA had stronger correlations with mortality.